Lupus
It's never Lupus
Lupus has made its way into popculture through various means, but in particular through the show House.MD, where it was used as a ‘red herring’ for the shows various medical mysteries, due to it presenting with a wide range of symptoms, though often it is not lupus. It’s never lupus. A running joke in the show, where lupus was used as a false diagnosis repeatedly, even resulting in a whole compilation of clips from the show, where it’s not lupus. Infact, this joke apparently helped raise awareness for lupus, which is how I came to learn about it. 1 Full disclosure I have only seen bits of the show so I don’t know of any underlying story going on in it.
What is Lupus
Lupus is a chronic autoimmune disease where the immune system mistakenly attacks healthy body tissue, causing inflammation & damage. Lupus is characterized by multisystem inflammation and production of auto-antibodies that bind to the body’s own antigens. Inflammation and autoantibodies can cause damage to any organ, but most often affect the skin, joints, blood cells, kidneys, and brain.2
There are four main types of lupus, each varying in severity and impact on the body:
Systemic Lupus Erythematosus (SLE) – The most common form, accounting for about 70% of lupus cases. In nearly half of these cases, major organs or tissues such as the heart, lungs, kidneys, or brain are affected.
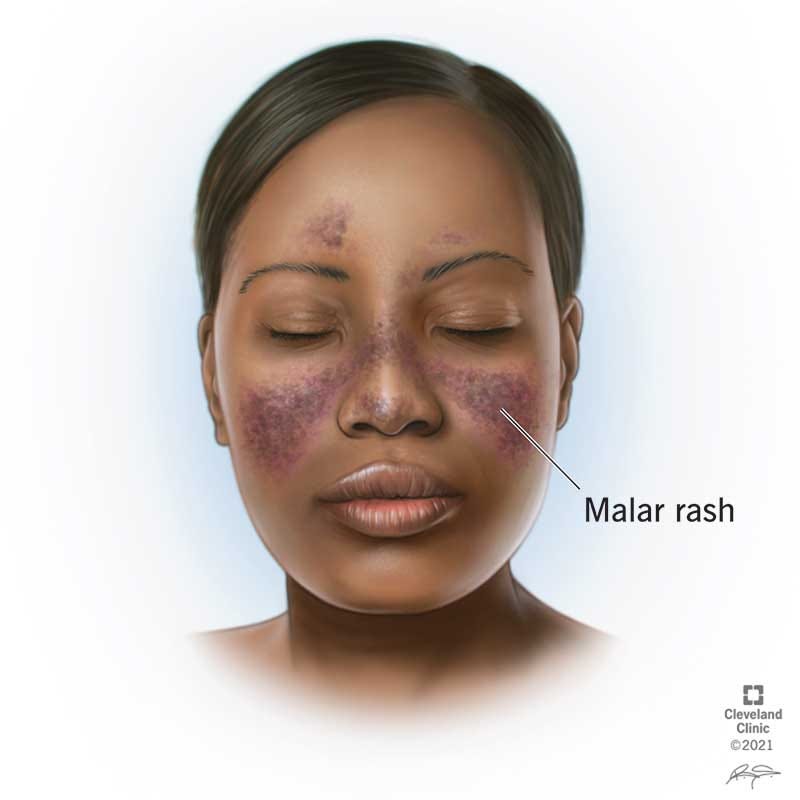
Cutaneous Lupus – Affects only the skin and makes up around 10% of lupus cases. It often presents as rashes or lesions, particularly after sun exposure.
Drug-Induced Lupus – Caused by prolonged use of certain medications, this form also accounts for roughly 10% of cases. Its symptoms resemble those of systemic lupus but usually resolve once the triggering medication is discontinued.
Neonatal Lupus – A rare condition in which a mother’s antibodies affect the fetus. Newborns may experience a temporary rash, liver issues, or low blood cell counts, but these symptoms typically disappear within six months without long-term effects. 3
Causes & Risk Factors
The exact cause of Lupus is unknown, though studies have found that there are a variety of factors causing Lupus. These include:
Genetic factors: Having certain genetic mutations may make you more likely to have lupus.
Hormones: Reactions to certain hormones in your body (especially estrogen) may make you more likely to develop lupus.
Environmental factors: Aspects about where you live and how much pollution or sunlight you’re exposed to might affect your lupus risk.
Your health history: Smoking, your stress level and having certain other health conditions (like other autoimmune diseases) might trigger lupus.4
Some risk factors include:
Gender: 90% of lupus patients are women.
Age: Commonly diagnosed between 15-45 years.
Ethnicity: 2 to 3 times more prevalent in African, Hispanic, Asian, and Indigenous populations. 5
The evidence for the causes of lupus points towards dysregulated apoptosis(DA), which leads to increased cell death. While DA itself cannot cause lupus, the fragments of dead cells are presented to the immune system in the form of their anti-gens(proteins on the cell surface membrane which identify them) In a healthy immune system, the body's own antigens are usually ignored. However, in lupus patients, genetic defects can lead to the development of intolerant lymphocytes that mistakenly react to the body’s own antigens. This triggers the production of auto-reactive T-cells and B-cells, resulting in the formation of autoantibodies and inflammatory factors. 6
The prefix ‘auto’ here refers to self, so an auto-antibody would be targeting the body’s cells and auto-reactive T-cells & B-cells are those which attack human body cells. While genetic factors underlie the background mechanism, the disease itself is typically triggered by environmental factors such as infections, drugs, or exposure to sunlight.

Symptoms
Symptoms for Lupus tend to present themselves as flare-ups, where the body goes through episodes of sickness where the symptoms suddenly worsen after a period of remission or mild disease activity.. These vary in severity, going from mild discomfort to a severe organ involvement that would require medical attentions. They can go on for as little as a few days to as long as several weeks.
There are various triggers for a lupus flare-up, such as:
Stress – Physical or emotional stress can weaken the immune system and increase inflammation.
Sunlight (UV Exposure) – Ultraviolet rays can trigger skin rashes and systemic inflammation.
Infections – Viral or bacterial infections can overstimulate the immune system, leading to increased lupus activity.
Hormonal Changes – Menstruation, pregnancy, or menopause may contribute to flare-ups.
Certain Medications – Drugs such as sulfa antibiotics or hormonal therapies may worsen symptoms.
Lack of Sleep & Poor Diet – Inadequate rest and an unhealthy diet can increase fatigue and inflammation. 7
The symptoms of a flare-up depend on the individual and can include:
Increased Fatigue – Feeling more exhausted than usual.
Joint Pain & Swelling – More intense stiffness and inflammation in joints.
Skin Rashes – Worsening of the characteristic butterfly rash or new skin issues.
Fever & Headaches – Low-grade fever and persistent headaches.
Chest Pain & Shortness of Breath – Inflammation affecting the heart or lungs.
Cognitive Issues – Memory fog, difficulty concentrating, or confusion.
In severe cases, lupus can lead to kidney inflammation (Lupus Nephritis), heart and lung complications, and neurological issues such as seizures or memory loss. 8
Diagnosis & Treatment
Diagnosis of lupus typically uses Anti-Nuclear Antibody (ANA) tests. These detect and identify the present of antibodies which target the nucleus/core of body cells. A positive test suggests and overactive immune system in 95% of tests, though this is not indicative of lupus since other conditions also present a positive ANA test. Further tests, such as anti-dsDNA and anti-Smith antibodies, help confirm a lupus diagnosis. Furthermore, the use of blood tests, urine analysis and biopsies of the skin & kidney can be also be used in the diagnostic process. 9
There are various treatments for Lupus which change depending on the symptoms presented. These include:
NSAIDs (Nonsteroidal Anti-Inflammatory Drugs): Over-the-counter options like ibuprofen and naproxen help manage pain, swelling, and fever. Prescription-strength versions are available but may cause stomach issues, kidney problems, or increased heart risks.
Antimalarial Drugs: Hydroxychloroquine (Plaquenil) helps control lupus symptoms and prevent flares. Rare side effects include stomach discomfort and potential retina damage, so regular eye exams are needed.
Corticosteroids: Medications like prednisone reduce inflammation, especially in severe cases. High doses can treat kidney or brain involvement but may cause weight gain, high blood pressure, osteoporosis, and increased infection risk.
Immunosuppressants: Drugs like methotrexate and azathioprine suppress the immune system in severe lupus cases. Side effects include infection risk, liver damage, and potential fertility issues.
Biologics: Belimumab (Benlysta) and rituximab (Rituxan) target specific immune responses. They may help when other treatments fail but can increase infection risk and, in rare cases, worsen depression.
New & Emerging Treatments: Voclosporin has shown promise in clinical trials, and other experimental drugs like abatacept and anifrolumab are being studied.
Managing lupus often requires a combination of medications, lifestyle changes, and regular medical monitoring.
Well that’s a wrap. It’s good to back after so long. till next time, adios